Lymphoedema: what you need to know
March is Lymphoedema Awareness Month, so we are sharing information for people who have had treatment for cancer and may be at risk of developing this condition.
What is lymphoedema?
Lymphoedema is swelling (oedema) that occurs when fluid (lymph) builds up in tissues, under the skin, or sometimes more deeply in the chest, abdomen or neck. Your arms and legs are most commonly affected after cancer treatment.
When this swelling is caused by damage to the lymphatic system (for example, by surgery or radiotherapy), it is called secondary lymphoedema. In rare cases, people may develop primary lymphoedema, but we are only discussing secondary lymphoedema here.
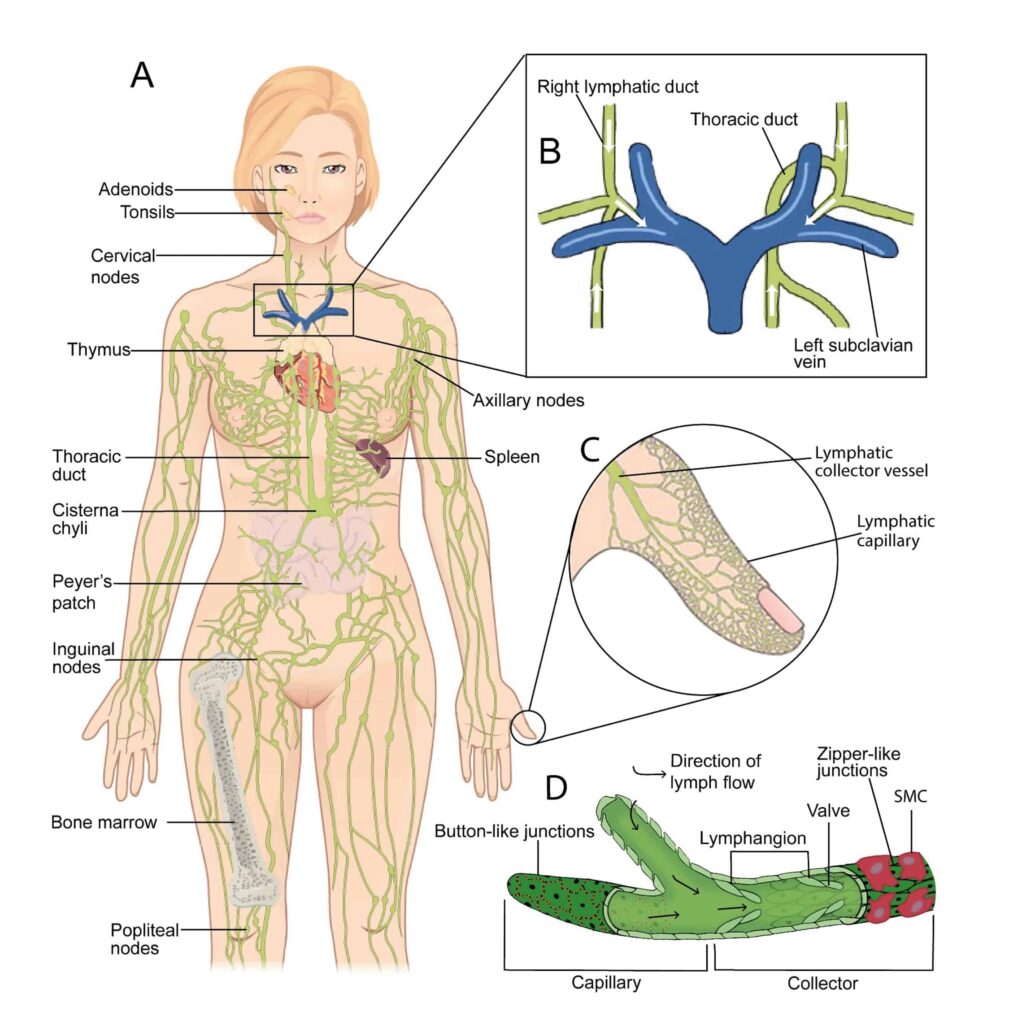
What is the lymphatic system?
The lymphatic system protects the body against infection. It is made up of a network of fine tubes across the body. It carries lymph fluid from tissues and organs and takes this to lymph nodes. The lymph nodes filter the lymph fluid removing bacteria and viruses. Then the filtered lymph fluid passes out of the lymph nodes into the bloodstream.
Who gets lymphoedema?
If the lymphatic system isn’t working properly, lymphoedema can occur at any time. For people diagnosed with cancer this can happen during initial treatment, after treatment is completed or when you’re in remission. It may develop if you’re experiencing advanced cancer. Usually it develops slowly, over many months or even years.

More than one in 5 people with cancer develop lymphoedema to some degree. Most don’t and it depends on the type of cancer you have, where it is, what treatment you’ve had and other health conditions you experience.
Risk factors include (from the Cancer Council, 2023):
- surgery that removes lymph nodes
- radiation therapy that damages the lymphatic system (scarring and thickening the vessels so they’re not carrying the lymph fluid as well as before)
- Taxane-based chemotherapy (speak with your oncologist about this association)
- an infection in the limb where lymph nodes were removed/damaged
- an injury to the lymphatic vessels
- obesity
- not being able to move around easily
- rheumatoid arthritis
- older age.
The table shows areas that may be affected by lymphoedema depending on the type of cancer:
| Cancer type | Commonly affected areas |
| Bladder | Genitals and legs |
| Breast | Arm, hand, breast, chest, trunk |
| Cervical | Genitals and legs |
| Head and neck | Face, below chin and/or neck |
| Melanoma | Any part of the body such as face, neck, hand, forearm, upper arm or whole arm, breast and/or chest wall, legs |
| Ovarian | Genitals, abdomen/trunk and legs |
| Uterine | Legs |
| Vulvar/vaginal | Genitals and legs |
How do I know I have lymphoedema?
Diagnosing lymphoedema early gives you the best chance of reducing how it affects you.
Early signs include:
- swelling that is soft to the touch and is usually not painful at first
- swelling and a heavy or achy feeling in your arms or legs that may spread to your fingers and toes
- swelling and a tight uncomfortable feeling on your face, neck, or under your chin
- difficulty moving your head or neck
- a dent when you press on the swollen area
- tight watches, jewellery or clothes.

Later signs include:
- swelling that doesn’t go down after elevation (overnight)
- swelling that is firmer and more difficult to dent
- infection – cellulitis (redness, heat and pain) of the skin over the swollen area
- nail changes to the affected limb.
What help can I get?
Treatment improves the lymphatic fluid’s flow through the affected area. This helps reduce swelling and improves the health of the swollen tissue. Reducing the swelling will lower your risk of infection, make movement easier and more comfortable, and improve your wellbeing. A range of health professionals may be involved in your care including a lymphoedema practitioner, your doctor, a podiatrist and dietitian.
Treatment can include:
- skin care, especially preventing infection, including nail care
- exercise, moving the affected area helps move the lymphatic fluid
- maintaining a healthy weight
- massage therapy (manual lymphatic drainage, if needed)
- compression therapy (if advised).

If you talk to your doctor about getting a Management Plan, you can be referred to an Accredited Lymphoedema Practitioner and may be eligible for Medicare rebates for up to five sessions from approved allied health professionals. You can also ask your oncology team about what services are available.
More information
Australasian Lymphology Association (ALA) (lymphoedema.org.au) The ALA is a professional association for lymphoedema practitioners and those working in or interested in lymphoedema. Their website includes information and a look-up tool to help you find an accredited practitioner near you.
Lymphoedema Association Australia (www.lymphaustralia.org.au) The Lymphoedema Association provides information and support to people living with lymphoedema.
Counterpart webinar recording: Lymphoedema (recorded 6 March 23)
Counterpart webinar recording: Self care for lymphoedema (recorded 9 March 22)
Understanding Lymphoedema (cancervic.org.au) (Cancer Council Victoria)
Physiotherapy and Lymphoedema (headandneckcancer.org.au) Information about lymphoedema as a result of head and neck cancer.
 Inherited Cancers, in partnership with Jean Hailes for Women’s Health, is launching the National Medically Induced Menopause Survey to help create the vital resources the community urgently needs. Medically induced menopause impacts many individuals managing ovarian cancer risk, yet accessing clear, relevant, Australia-specific information remains a challenge.
Inherited Cancers, in partnership with Jean Hailes for Women’s Health, is launching the National Medically Induced Menopause Survey to help create the vital resources the community urgently needs. Medically induced menopause impacts many individuals managing ovarian cancer risk, yet accessing clear, relevant, Australia-specific information remains a challenge. The FOCUSau study, lead by Melbourne University is recruiting individuals living with advanced cancer and their family carers to evaluate a three-month online support program designed to enhance their wellbeing and quality of life. Participants will work through four guided sessions together over three months. The study will compare those who complete the program with those who do not, with participation in the program being randomly assigned. Both groups will continue receiving usual care from their healthcare team. Participants will complete surveys at the start and end of the study to assess whether the FOCUSau program leads to improvements in wellbeing and quality of life.
The FOCUSau study, lead by Melbourne University is recruiting individuals living with advanced cancer and their family carers to evaluate a three-month online support program designed to enhance their wellbeing and quality of life. Participants will work through four guided sessions together over three months. The study will compare those who complete the program with those who do not, with participation in the program being randomly assigned. Both groups will continue receiving usual care from their healthcare team. Participants will complete surveys at the start and end of the study to assess whether the FOCUSau program leads to improvements in wellbeing and quality of life. Western Sydney University (WSU) is looking for participants for a study on how Indian Australian cancer patients cope with their diagnosis. By completing an online survey, you’ll answer questions about your background, how you manage stress, and how effective these strategies are. At the end of the survey, you can choose to participate in an interview. The findings from this study will help researchers better understand how Indian Australians cope with cancer, which could lead to improvements in healthcare for those facing cancer in this community.
Western Sydney University (WSU) is looking for participants for a study on how Indian Australian cancer patients cope with their diagnosis. By completing an online survey, you’ll answer questions about your background, how you manage stress, and how effective these strategies are. At the end of the survey, you can choose to participate in an interview. The findings from this study will help researchers better understand how Indian Australians cope with cancer, which could lead to improvements in healthcare for those facing cancer in this community.
 This pre-conference workshop, co-hosted by Breast Cancer Network Australia (BCNA) and the Clinical Oncology Society of Australia (COSA), offers participants the opportunity to enhance their understanding of consumer engagement in cancer care. Through interactive sessions, attendees will learn about the fundamentals of consumer engagement, including its role in health policy, research, and strategy. Participants will gain practical skills in meaningful engagement, from recruitment and ethical considerations to co-design practices. The workshop will also cover how to measure impact and sustain long-term engagement in cancer care.
This pre-conference workshop, co-hosted by Breast Cancer Network Australia (BCNA) and the Clinical Oncology Society of Australia (COSA), offers participants the opportunity to enhance their understanding of consumer engagement in cancer care. Through interactive sessions, attendees will learn about the fundamentals of consumer engagement, including its role in health policy, research, and strategy. Participants will gain practical skills in meaningful engagement, from recruitment and ethical considerations to co-design practices. The workshop will also cover how to measure impact and sustain long-term engagement in cancer care. The Leukaemia Foundation offers several ways for you to connect with others, learn more about blood cancer, and hear from healthcare professionals. Their online support groups, education webinars, and private Facebook groups are moderated by Leukaemia Foundation staff and are open to anyone living with blood cancer, as well as their family and friends, across Australia. No matter where you live, your age, or the stage of blood cancer, you’re welcome to join. These webinars, seminars, and support groups are easy to access via Zoom – all you need is a device such as a smartphone, computer, or laptop and an internet connection.
The Leukaemia Foundation offers several ways for you to connect with others, learn more about blood cancer, and hear from healthcare professionals. Their online support groups, education webinars, and private Facebook groups are moderated by Leukaemia Foundation staff and are open to anyone living with blood cancer, as well as their family and friends, across Australia. No matter where you live, your age, or the stage of blood cancer, you’re welcome to join. These webinars, seminars, and support groups are easy to access via Zoom – all you need is a device such as a smartphone, computer, or laptop and an internet connection.